HELA CELLS
|
HeLa cells are a population of cells that were established after cells were taken from a women named Henrietta Lacks, a working-class African-American woman living near Baltimore, in 1951 when she had visited the doctor's office complaining about a lump in her cervix.
When the doctors took a biopsy of the tumour, they realized that the cells grew at an incredible pace and unlike other cell cultures, survived for longer amounts of time. Extra cells were taken without the knowledge or permission of her or her family as they were the first human cells to grow well in a lab and these cells were grown in vitro by a researcher named Dr. George Gey. After more than 50 years, there are now billions and billions of HeLa cells in laboratories all over the world. It's the most commonly used cell line, and it's known to be extremely resilient. |
|
Impact of HeLa cells on scientific discoveries:
- Helped scientists develop a vaccine for polio
- Gone into space to be exposed to nuclear testing and toxins as an experiment to see what happens to human cells if humans were to venture into space
- Furthered understanding on cancer and HIV/AIDS cells
- Still widely used today to grow viruses and to test anti-tumor medications
Ethical and moral questions about hela cells
Should patients' identities be protected? |
As researchers thought that the identity of the person the cells came from should be kept private, they decided to name the cell line HeLa to maintain anonymity. However, many people at the time thought that the cells came from a woman named Helen Lane (as well as other variations). Because Henrietta's cells were taken without knowledge from her or her family, when her cells became widespread, no one in Henrietta's family knew what was going on. |
Should patients need to give consent? |
Neither Henrietta or her family gave consent for her cells to be taken in the first place and used this way. Not only that but the family never understood how the cells would be used as it wasn’t explained to them. This led to a lot of anxiety and strain for the family. The issue of consent is still widely debated. |
Should companies be able to profit off of someone's cultured cells? |
Henrietta Lacks did receive free healthcare treatment for her cervical cancer, but because she was African American, she had to travel miles to a segregated hospital to be treated. George Gey, the doctor who treated Henrietta Lacks, didn’t profit from the cells when he sent them to other scientists, but some pharmaceutical businesses cultured HeLa cells and have profited from their manufacture. While big companies are making money off Henrietta's cells, her family is unable to afford for healthcare in the USA. |
Tuskegee syphyllis STudy
|
|
The Public Health Service and the Tuskegee Institute worked together in 1932 began a study to record the natural history of syphilis in hopes of justifying treatment programs for blacks. It was called the “Tuskegee Study of Untreated Syphilis in the Negro Male.”
The study initially involved 600 black men: 399 with syphilis, 201 who did not have the disease. The study was conducted without patients’ informed consent. Researchers told the men they were being treated for “bad blood,” which was a local term used to describe several illnesses, including syphilis, anemia, and fatigue. In truth, they did not receive the proper treatment needed to cure their illness. In exchange for taking part in the study, the men received free medical exams, free meals, and burial insurance. Although the study was originally supposed to last 6 months, the study actually went on for 40 years. |
ETHICAL ISSUES REGARDING THE TUSKEGEE STUDY
In July 1972, an Associated Press story about the Tuskegee Study caused a public outcry that led the Assistant Secretary for Health and Scientific Affairs to appoint an Ad Hoc Advisory Panel to review the study. The panel had nine members from the fields of medicine, law, religion, labor, education, health administration, and public affairs.
The panel had found that, even though the men had freely agreed to proceed with the examination and treatment, there was no evidence that researchers had informed them of the study or its real purpose. In fact, the men had been misled and had not been given all the facts required to provide informed consent. The men were never given adequate treatment for their disease. Even when penicillin became the drug of choice for syphilis in 1947, researchers did not offer it to the subjects. The advisory panel found nothing to show that subjects were ever given the choice of quitting the study, even when this new, highly effective treatment became widely used.
The advisory panel concluded that the Tuskegee Study was “ethically unjustified”– the knowledge gained was sparse when compared with the risks the study posed for its subjects. In October 1972, the panel advised stopping the study at once.
The panel had found that, even though the men had freely agreed to proceed with the examination and treatment, there was no evidence that researchers had informed them of the study or its real purpose. In fact, the men had been misled and had not been given all the facts required to provide informed consent. The men were never given adequate treatment for their disease. Even when penicillin became the drug of choice for syphilis in 1947, researchers did not offer it to the subjects. The advisory panel found nothing to show that subjects were ever given the choice of quitting the study, even when this new, highly effective treatment became widely used.
The advisory panel concluded that the Tuskegee Study was “ethically unjustified”– the knowledge gained was sparse when compared with the risks the study posed for its subjects. In October 1972, the panel advised stopping the study at once.
NAZI MEDICAL EXPERIMENTS
|
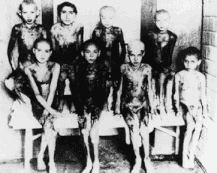
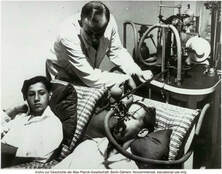
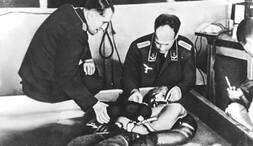
During World War II, a number of German physicians conducted painful and often deadly experiments on thousands of prisoners without their permission.
Many experiments in the camps were used to determine the survival of Axis military personnel in the field. For example, physicians from the German air force and from the German Experimental Institution for Aviation conducted high-altitude experiments on prisoners to determine the maximum altitude from which crews of damaged aircraft could parachute to safety. Scientists there also carried out so-called freezing experiments on prisoners to find an effective treatment for hypothermia. Prisoners were also used to test various methods of making seawater drinkable. Not only that, but the prisoners were used to test new drugs and to test immunization compounds and antibodies for the prevention and treatment of contagious diseases, including malaria, typhus, tuberculosis, typhoid fever, yellow fever, and infectious hepatitis. |
NUREMBURG CODE
Considering the inhumane conditions, lack of consent, and questionable research standards, modern scientists overwhelmingly reject the use of results from experiments in the camps. The Nuremberg Code was created In the aftermath of the discovery of the camp experiments and subsequent trials to address abuses committed by medical professionals during the Holocaust. The Nuremberg Code included the principle of informed consent and required standards for research.